Things to know about vaginal pain and vulvodynia
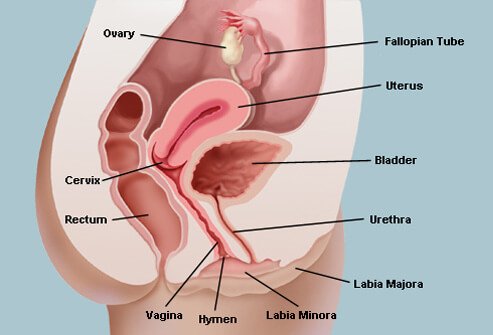
Illustration of Vagina
- Vulvodynia (vaginal pain) refers to pain in the area of the vulva and vaginal opening for which no cause can be identified.
- Vulvodynia is not related to sexually transmitted diseases (STDs).
- The exact cause of vulvodynia is not known.
- Symptoms include a burning, throbbing, or aching pain that can be localized to one area of the vulva or more widespread.
- Vaginal itching may be associated with vulvodynia.
- Vulvodynia can be treated with medications and/or self-care (home remedy) measures. No one treatment is effective for all women.
- Local anesthetics, local estrogen creams, antidepressants, and anticonvulsive drugs are examples of medical treatments for vulvodynia.
- Biofeedback, exercises, and nerve blocks may benefit other women.
- Vulvodynia is not associated with cancer or serious medical conditions, but it can be a source of long-term physical and emotional discomfort.
What is vaginal pain (vulvodynia)?
Vulvodynia refers to pain in the area of the vulva and vaginal opening. Vulvodynia is considered pain for which there is no known cause. It is different from the pain that is located deep in the pelvis or internally in the vagina. This article focuses on pain in the vulvar region and at the opening (introitus) of the vagina. Deeper vaginal pain can also occur due to infections, tumors, and conditions that cause more generalized pain in the pelvic organs.
- Vaginal pain can be chronic and can last for years in some women.
- The degree of severity varies among women.
- It often occurs in the absence of physical signs or visible abnormalities.
- It can be severe and can interfere with sexual activity and cause painful intercourse (dyspareunia).
- However, there are several other causes of vaginal pain during or after sex.
Vaginal Pain Symptoms
Pain in the vagina or the female external genital organs (the vulva, which includes the labia, clitoris, and entrance to the vagina) most commonly is a result of infection. Vaginitis is another term for infection of the vagina. Yeast infection (Candida) is a particularly common form of vaginitis. Women are at increased risk for yeast vaginitis if they take antibiotics or cortisone medications, during pregnancy, and if their immune systems are suppressed by medications or disease. Vaginal pain can also be a result of injury or trauma to the vagina or vulva. Vaginal pain during sexual intercourse is referred to as dyspareunia. The medical term for vaginal pain is vulvodynia.
What are the signs and symptoms of vaginal pain?
The pain of vulvodynia can be debilitating and interfere with daily activities and sexual intercourse. It can make women feel a loss of control of their bodies, causing profound emotional and physical discomfort.
Symptoms of vulvodynia and vaginal pain may include:
- Burning or stinging pain in the vulva or vaginal opening
- Sharp, aching, or throbbing pain in the vagina or vulva
- Vaginal itching, sometimes with pain
- Pain that is constant or comes and goes
- Pain that occurs during sex or exercise
Some women report pain that is localized to one side or one area of the vulva, while others have more generalized and widespread pain. Usually, no physical signs or changes occur in and around the vagina with vulvodynia; however, sometimes the skin may be inflamed.
What if you have vaginal pain during pregnancy?
Vaginal pain may occur during the third trimester of pregnancy due to an increase in pressure on the cervix. Women who experienced vulvodynia before becoming pregnant may continue to experience this symptom during pregnancy.

SLIDESHOW
Female Sexual Dysfunction: Treatment for Women’s Sexual Disorders See Slideshow
What causes vaginal pain?
It is unclear why some women develop vulvodynia. It is not thought to be related to sexually transmitted diseases (STDs), although some women with vulvodynia have had multiple STDs.
Some theories suggest that vulvodynia may be related to:
- damage or irritation of nerves,
- abnormal responses to irritation or inflammation,
- allergic reactions,
- muscle spasms,
- a history of sexual abuse, or
- frequent use of antibiotics.
Familial or genetic factors also have been suggested to play a role in vulvodynia. Unfortunately, the exact cause has not been determined and most women have no known contributing factors.
What are risk factors for vaginal pain? Who gets it?
Since the cause is poorly understood, it is difficult to predict who is at risk for vulvodynia.
- It can affect women of all ages and races.
- It can begin as early as adolescence and can occur both before and after menopause.
- It may occur during the menstrual period or independent of the menstrual period.
Latest Women’s Health News
Daily Health News
Trending on MedicineNet
What exams and procedures can diagnose the cause of vaginal paint?
No specific tests confirm vulvodynia. Usually, vaginal pain and vulvodynia are diagnosed based on the characteristic symptoms of the condition. However, since vulvar and vaginal infections, (for example, yeast infections, bacterial vaginosis, and vaginitis) are associated with vaginal burning and itching, cultures or other diagnostic tests may be ordered to rule out vaginal infections.
What is the treatment for vaginal pain and vulvodynia? Can the condition be cured?
Vulvodynia is a chronic condition (it may last for months to years) in some women; in others, it may come and go. Vulvodynia and vaginal pain can be managed using medical treatments and self-care (home remedies). Not all treatments will be effective for every woman, and a woman may have to try different treatments to find the most effective option for her.
Vulvodynia is not associated with cancer or with any serious medical diseases, but it may be a source of chronic pain and emotional discomfort for some women.

IMAGES
Vaginal Pain See a medical illustration of the female vagina plus our entire medical gallery of human anatomy and physiology See Images
What medications and home therapies can relieve vaginal pain?
Some of the medications that have been useful include:
Other medical therapies for women with severe vulvodynia include:
- Injections of interferon or nerve blocks, in which medications are injected to reduce signals from nerves in the affected areas
- Biofeedback training and pelvic floor exercises have been helpful for some women.
- Surgical removal of affected tissue can be of benefit in women with vulvodynia due to vulvar vestibulitis syndrome, a particular type of vulvodynia that is located in the area of the hymenal ring.
Subscribe to MedicineNet’s General Health Newsletter
By clicking Submit, I agree to the MedicineNet’s Terms & Conditions & Privacy Policy and understand that I may opt out of MedicineNet’s subscriptions at any time.
What treatments and home remedies help relieve pain?
Home remedies and self-care measures for vulvodynia can bring relief to many women.
Some self-care measures to relieve the pain of vulvodynia include:
- Rinsing the area with cool water, particularly after urination and sexual activity
- Soaking in cool or warm sitz baths
- Using topical ice packs wrapped in a towel
- Heating pad use, in contrast, may help some women
- Using mild, unscented soaps and detergent
- Using white, unscented toilet tissue
- Wearing white cotton underwear
- Wearing loose-fitting clothing and avoiding stockings or pantyhose
- Avoiding pools or hot tubs with chlorinated water
- Using a water-soluble lubricant during sexual intercourse
- Avoiding activities such as bicycling, that put pressure on the vulvar area
- Keeping the vulvar area dry and clean
- Avoid food that can make the urine more irritating to the skin of the genital area, such as beans, berries, nuts, and chocolate
- Over-the-counter antihistamines can help reduce itching, particularly at night
Medically Reviewed on 4/27/2022
References
Gunther, E. S. “Clinical manifestations and diagnosis of generalized vulvodynia.” UpToDate. Updated: Oct 03, 2017.
<https://www.uptodate.com/contents/clinical-manifestations-and-diagnosis-of-generalized-vulvodynia>