Things to know about gonorrhea in women
Gonorrhea is a bacterial infection transmitted during sexual contact.
- Gonorrhea is a bacterial infection that is transmitted during sexual activity.
- Gonorrhea is not transmitted from toilet seats.
- Women infected with gonorrhea may not have any symptoms. Common gonorrhea symptoms and signs include vaginal discharge and pain when a woman urinates.
- Gonorrhea is treated with antibiotics.
- Gonorrhea may cause pelvic inflammatory disease (PID), tubo-ovarian abscess, and infertility.
What is gonorrhea? How do you get it?
Gonorrhea is a bacterial infection caused by the organism Neisseria gonorrhoeae that is transmitted during unprotected sex. It is one of the oldest known sexually transmitted diseases. Among individuals who are infected with gonorrhea, 50% to 70% also will be infected with chlamydia, another type of bacteria that causes another STD.
Contrary to popular belief, gonorrhea cannot be transmitted from toilet seats or door handles.
- The bacterium that causes gonorrhea requires very specific conditions for growth and reproduction. It cannot live outside the body for more than a few seconds or minutes, nor can it live on the skin of the hands, arms, or legs.
- It survives only on moist surfaces within the body and is found most commonly in the vagina, and, more commonly, the cervix (the end of the uterus that protrudes into the vagina).
- It can also live in the tube (urethra) through which urine drains from the bladder.
- Neisseria gonorrhoeae can even exist in the back of the throat (from oral sex) and in the rectum (from anal sex).

Oral Gonorrhea Symptoms
Many people, especially young teens, consider oral sex to be “safe” sex. “Safe sex” by many people is defined as having sexual gratification by means that reduces or eliminates the chance of producing a fetus (pregnancy). However, many people include in the meaning of “safe sex,” sex practices that prevent or significantly reduce the possibility of getting a disease from a sex partner for examples:
- HIV,
- chlamydia,
- syphilis, or
- gonorrhea.
Most doctors do not consider oral (and other) sexual practices “safe” unless precautions are taken to prevent or substantially reduce disease transmission between partners, or if the sex partners are uninfected.
What are STDs and how do you prevent them?
Sexually transmitted diseases (STDs) are infections that can be transferred from one sexual partner to another through any type of sexual contact. STDs are sometimes referred to as sexually transmitted infections (STIs) since they involve the transmission of a disease-causing organism from one person to another during sexual activity. It is important to realize that sexual contact includes more than just sexual intercourse (vaginal and anal). Sexual contact includes kissing, oral sex, and the use of sexual “toys,” such as vibrators.
STDs probably have been around for thousands of years, but the most dangerous of these conditions, the acquired immunodeficiency syndrome (AIDS) was first recognized in 1981, and the causative human immunodeficiency virus (HIV), was first identified in 1984.
Many STDs are treatable, but effective cures are lacking for others, such as HIV, HPV (human papillomavirus), and possibly hepatitis B. Even gonorrhea, once easily cured, has become resistant to many of the older traditional antibiotics. Many STDs can be present in, and spread by, people who do not have any symptoms of the condition and have not yet been diagnosed with an STD. Therefore, public awareness and education about these infections and the methods of preventing them are important.
There is no such thing as “safe” sex. The only truly effective way to prevent STDs is abstinence. Sex in the context of a monogamous relationship wherein neither party is infected with an STD also is considered “safe.” Most people think that kissing is a safe activity. Unfortunately, syphilis, herpes, and other infections can be contracted through this relatively simple and harmless act. All other forms of sexual contact carry some risk.
Condoms are commonly thought to protect against STDs. While condoms are useful in decreasing the spread of certain infections, such as chlamydia and gonorrhea, they do not fully protect against other infections such as genital herpes, genital warts, syphilis, and AIDS. Prevention of the spread of STDs is dependent upon the counseling of at-risk individuals and the early diagnosis and treatment of infections.

SLIDESHOW
12 Preventable STDs: Pictures, Symptoms, Diagnosis, Treatment See Slideshow
What are the early symptoms signs and of gonorrhea? What symptoms develop later?
Most infected women have no symptoms, especially in the early stages of the infection.
Gonorrhea symptoms and signs include:
- Burning
- Frequent, and/or painful urination
- Yellowish vaginal discharge
- Redness and swelling of the genitals
- Burning or itching of the vaginal area
- Sore throat
Untreated gonorrhea can lead to a severe pelvic infection with inflammation of the Fallopian tubes and ovaries. Gonorrheal infection of the Fallopian tubes can lead to a serious, painful infection of the pelvis known as pelvic inflammatory disease or PID. PID occurs in many women with gonorrheal infections of the uterine cervix. Symptoms of pelvic infection include fever, pelvic cramping, pelvic pain, or pain with intercourse.
Pelvic infection can lead to difficulty in becoming pregnant or even infertility because of tubal damage or obstruction. Occasionally, if the infection is severe enough, a localized area of infection and pus-like discharge (an abscess) form (tubo-ovarian abscess) that can be life-threatening, and major surgery may be necessary.
Gonorrhea infections in people with conditions causing seriously depressed immune function, such as AIDS or immunosuppressive treatments, can be even more serious.
Latest Sexual Health News
Daily Health News
Trending on MedicineNet
How is gonorrhea diagnosed?
Testing for gonorrhea is done by swabbing the infected site (rectum, throat, cervix) and identifying the bacteria in the laboratory either through culturing of the material from the swab (growing the bacteria) or identification of the genetic material from the bacteria. Sometimes the tests do not show bacteria because of sampling errors (the sampled area does not contain bacteria) or other technical difficulties, even when the woman has an infection.
Newer tests to diagnose gonorrhea involve the use of DNA probes or amplification techniques (for example, polymerase chain reaction, or PCR) to identify the genetic material of the bacteria. These tests are more expensive than cultures but typically yield more rapid results.
What are the treatments for gonorrhea? Can gonorrhea be cured?
In the past, the treatment of uncomplicated gonorrhea was fairly simple. A single injection of penicillin cured almost every infected person. Unfortunately, there are new strains of gonorrhea that have become resistant to various antibiotics, including penicillins, and are therefore more difficult to treat. Fortunately, gonorrhea can still be treated by other injectable or oral medications.
Uncomplicated gonococcal infections of the cervix, urethra, and rectum, are usually treated by a single injection of ceftriaxone intramuscularly or by cefixime (Suprax) in a single oral dose. For uncomplicated gonococcal infections of the pharynx, the recommended treatment is ceftriaxone in a single IM dose.
Alternative regimens for uncomplicated gonococcal infections of the cervix, urethra, and rectum is spectinomycin in nonpregnant women (not available in the United States) in a single IM dose or single doses of cephalosporins (ceftizoxime or cefoxitin, administered with probenecid (Benemid), or cefotaxime).
Treatment should always include medication that will treat chlamydia, for example, azithromycin (Zithromax, Zmax) or doxycycline (Vibramycin, Oracea, Adoxa, Atridox, and others), as well as gonorrhea because both diseases frequently exist together in the same person. The sexual partners of women who have had either gonorrhea or chlamydia must receive treatment for both infections since their sex partners may be infected as well. Treating the sex partners also prevents reinfection of the woman.
Women suffering from PID require more aggressive treatment that is effective against the bacteria that cause gonorrhea as well as against other organisms. These women often require hospitalization and intravenous administration of antibiotics.
It is important to note that doxycycline, one of the recommended drugs for the treatment of PID, is not recommended for use in pregnant women.
Gonorrhea is one of the easier STIs to prevent because the bacterium that causes the infection can survive only under certain conditions. The use of condoms protects against infection. Since the organism can live in the throat, condoms should be used during oral-genital contact as well.
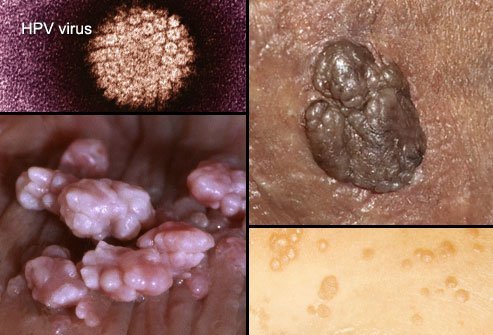
IMAGES
Gonorrhea In Women See pictures of sexual conditions and sexually transmitted diseases (STDs) See Images
Medically Reviewed on 4/22/2022
References
“Current Concepts in Bacterial Sexually Transmitted Diseases.”
Bong Suk Shim.
“Chlamydial infection increases gonococcal colonization in a novel murine coinfection model”
Rachel A. Vonck et al
“Pelvic inflammatory disease”
National Institute of Allergy and Infectious Diseases
United States. Centers for Disease Control and Prevention. “Gonorrhea — CDC Fact Sheet.” June 2017. <https://www.cdc.gov/std/gonorrhea/Gonorrhea-FS-June-2017.pdf<.